Strokes pose a challenge in diagnosis and require time-sensitive treatment. Ischemic stroke, an interruption of blood flow to part of the brain, and hemorrhagic stroke, bleeding from a blood vessel within the brain, can both cause a range of debilitating symptoms including speech difficulties, weakness, numbness, visual loss, trouble walking and changes in cognition. Due to the array of possible stroke symptoms, there are many conditions that can be mistaken for stroke, also known as a stroke ‘mimics.’ Rapidly recognizing these diagnoses and differentiating them from true strokes is critical to avoiding misdiagnosis and preventing harm to patients.
Full Code is a medical simulation that allows you to hone your diagnostic skills in a virtual environment. Learn to differentiate strokes and stroke mimics with Full Code. Try a free case today!
Hypoglycemia
Among the most common and reversible stroke mimics is hypoglycemia or low blood sugar. Low blood sugar can cause a sudden change in speech, including slurred or confused speech, which can easily be mistaken for a stroke. Severe hypoglycemia can cause decreased mental status and confusion which can make examination difficult. Thus, a robust stroke treatment protocol includes the immediate assessment of blood sugar, typically via a ‘fingerstick’ blood glucose test. This can be rapidly done en route to the hospital or on arrival. If recognized, immediate reversal using oral glucose gel or intravenous dextrose may rapidly correct the neurological symptoms avoiding a complex and wasteful medical evaluation.
Other electrolyte or metabolic problems, such as acute kidney failure, high calcium levels, liver dysfunction and thyroid abnormalities can also contribute to symptoms that may be mistaken for a stroke.
Brain Mass (Tumor)
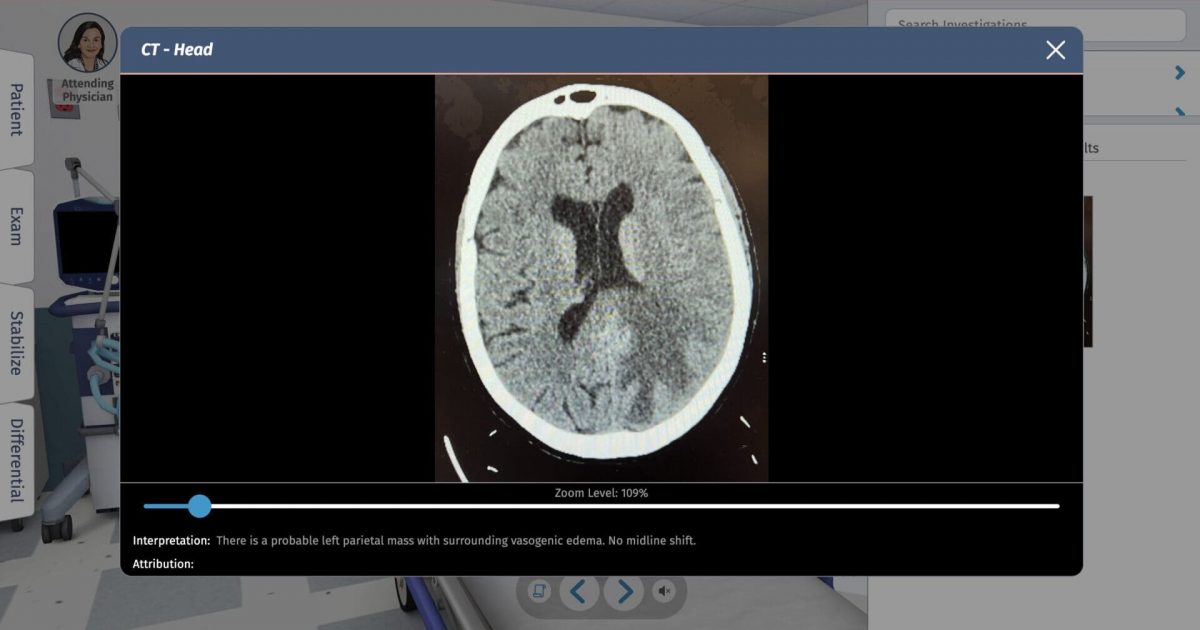
Brain masses (or tumors) comprise a large group of diagnoses that include primary neoplasms (originating from the brain) and metastatic lesions (spreading from another site). Primary brain tumors are classified based on the cell of origin and the aggressiveness of growth. The most common metastatic brain lesions originate from breast cancer, lung cancer or melanoma. Depending on the location of the tumor, brain masses can produce symptoms from direct invasion or local compression of areas of the brain as well as increased intracranial pressure. Symptoms can include cognitive or psychiatric changes, weakness, vision abnormalities, sensory deficits, gait difficulties, hallucinations and seizures. Headache is the most common initial presenting symptom. Symptoms are generally gradual in onset and progressive; however, rapid progression can occur due to herniation or CSF obstruction. CT as well as MRI imaging can help differentiate a brain tumor from a stroke.
Seizure
Seizures can cause residual neurological symptoms that may appear similar to a stroke. In the post-ictal phase of a seizure, patient’s may display focal weakness that mimics a stroke. This is known as a Todd paralysis. If the seizure episode was not witnessed, patient’s displaying these symptoms may be misdiagnosed as having an acute stroke, undergoing unnecessary testing and even treatment, such as tPA administration. Of note, seizure can also occur at the onset of an acute stroke, further complicating the ability to differentiate between strokes and this stroke mimic.
Bell’s Palsy
Facial nerve palsy, also known as Bell’s palsy, is a problem in the peripheral nerve innervating movement of the face. Bell’s palsy can cause a “facial droop” that can commonly be mistaken for a stroke. Unlike Bell’s palsy which may involve the forehead and eyelid, a facial droop caused by a stroke typically involves the lower half of the face (sparing the forehead). Sudden onset of facial droop or associated neurological symptoms in other areas of the bodies, should raise the level of concern for a stroke causing the facial droop. Testing for Lyme disease is an important consideration as this is a potential cause of Bell’s palsy. Once confirmed, treatment of Bell’s palsy involves the use of steroids and antivirals. Clinicians need to be familiar with the diagnosis and evaluation of Bell’s palsy in order to avoid inappropriate and wasteful neurological work-ups and stroke alert activations.
Migraine Headache
A migraine headache may be preceded by an aura — focal neurological symptoms accompanying a migraine headache, most commonly visual symptoms. However sensory or motor auras can easily be confused with a stroke. Some patients can experience an aura without headache which can raise the level of concern for a possible transient ischemic attack (TIA) or stroke. A ‘complex migraine’ can be difficult to differentiate from a true stroke. They may occur in younger patients, be associated with headache and may demonstrate resolution of symptoms with treatment of the headache. However, without a prior history of these events, the concern for a true stroke should remain high to avoid misdiagnosis and delay in critical treatment with tPA, thrombectomy or other intervention in the event of an ischemic stroke.
Peripheral Vertigo
Vertigo, an uncomfortable and sometimes debilitating spinning sensation can originate from the inner ear (peripheral vertigo) or from the brain (central vertigo). Peripheral vertigo is much more common and usually responds will to rest and medication. However, it can be challenging to consistently differentiate this from central vertigo, which can be due to a stroke. Vertigo can be caused by a posterior circulation stroke and so a high level of suspicion must be maintained. Neuroimaging may be necessary to differentiate the cause and avoid a missed diagnosis of acute stroke.
Multiple Sclerosis
Multiple sclerosis (MS) and other neurological conditions can also cause focal neurological symptoms that appear similar to a stroke. MS is a demyelinating autoimmune condition that causes damage to the central nervous system. Visual symptoms are common including including visual loss or double vision (diplopia) are common symptoms and MS can also cause loss of sensory or motor function. Symptoms more commonly present in young adulthood with gradual onset neurological symptoms. MRI imaging and lumbar puncture can help make the diagnosis and differentiate these symptoms from a true stroke.
**
As you can see, there are many related diagnoses to learn about in order to hone your recognition of strokes! Rapidly distinguishing between suspected stroke and stroke mimics is a key diagnostic skill for clinicians. Appropriate and rapid recognition of true strokes saves lives and prevents significant disability. Moreover, careful differentiation of stroke mimics prevents unnecessary stroke alert activations, saves resources and decreases unnecessary testing. Familiarity with the most common stroke mimics and stroke syndromes is the key to correct diagnosis.